Sameera Mushtaq1*
1*Lecturer, University Institute of Physical Therapy (UIPT) University of Lahore, Pakistan![]()
ABSTRACT
Background of the study: Urinary incontinence is a physically challenging and socially incapacitating situation with a loss of self-confidence. This study aims to narrate the latest literature on the efficacy of novel exercise-based techniques to treat stress urinary incontinence except the traditional exercise using Kegel’s method.
Methodology: The electronic searching was done using Google Scholar, Cochrane Library, PubMed, Science Direct, and BMC journals for the latest available at least three articles, including novel exercise regimes to treat stress urinary incontinence. The included techniques are Pilates, Paula Method, and the abdominal Hypopressive exercise technique. All the articles were analyzed, and their results are compiled in tabulated form in this narrative review.
Results: All the approaches like Pilates, Paula, and Hypopressive abdominal exercises are effective for the treatment of stress urinary incontinence. None of the regimes was found to be completely ineffective; however, the range of usefulness may vary.
Conclusion: This study asserts the ideology of inclusion of new therapies into clinical practice keeping in mind their latest literature-based evidence.
Keywords: Urinary incontinence, stress, exercise movement techniques, female, urinary incontinence epidemiology, pelvic floor.

Introduction
Urinary incontinence is a prevalent chronic illness affecting both males and females across the globe. It is a physically debilitating and socially incapacitating situation with a loss of self-confidence. Several large-scale studies have focused on the epidemiology of urinary incontinence (UI) in women in Western countries. According to the National Health and Nutrition Examination Study conducted on the data of the population residing in the United States, the prevalence of stress urinary incontinence SUI) was 45.9% which was the highest among other subtypes1. Various large-scale studies have also been conducted in Central and Eastern European countries. In this context, the LUTS Poland survey concluded that the prevalence of urinary incontinence was 14.6–25.4% among Polish adults aged ≥ 40 years2. In Shanxi, China, the latest study was conducted to estimate the prevalence of Stree Urinary incontinence in the adult female Chinese population and it was around 33.5%3. The Asian female population differs from the Western population both constitutionally and ethnically. A study focusing on the female population of Gulf countries described that the prevalence of UI was assessed to be around 20.3% to 54.5%4 .In another study conducted on women residing in Riyadh, Saudi Arabia 47.5% of females were diagnosed with UI, of which 79% cases were eliciting SUI symptoms. This study also highlighted an important factor that urinary incontinence can also have a vital impact on the religious acts and sexual relationships of these women5 .Due to the embarrassing nature of the problem, it is least reported by females to doctors. In Punjab (Pakistan), an observational study estimated the prevalence of UI of any type in Pakistani women. They concluded that mixed urinary incontinence (MUI) was most prevalent (64.45%); however, Stress UI and Urge UI came later with 29.59% and 5.96%, respectively6.Stress urinary incontinence has distressed various aspects of life, such as relationships, emotional health, sleep, work productivity, depression, and general health-related quality of life (HRQOL)7. The International Continence Society (ICS) outlines urinary incontinence (UI) as the patient complains of involuntary seepage or leakage of urine. 8 Stress urinary incontinence (SUI) comes under the umbrella term of Urinary incontinence. It can be further explained as the spontaneous loss of urine via the urethra specifically when the intravesical pressure surpasses the maximum urethral pressure9. SUI is a highly treatable as well as curable medical condition in some patients. There are many exercise-based interventions for treating SUI, like pelvic floor muscle exercises (Kegels), the Pilates method, deep abdominal muscle training, Hypopressive exercises, the Paula method, yoga training, and others. Among these techniques, Kegels has the most robust evidence of its effectiveness10. Kegels, or pelvic floor muscle training, was first proposed in 1948 by an American gynecologist named Arnold Henry Kegel. Later, this technique was named after him. Kegel proved the effects of regular and precise pelvic floor muscle training by conducting a trial of 500 patients, of which around 84% were cured of urinary incontinence11. This is now further confirmed by many clinical trials that have evaluated the effectiveness of Kegels on urinary incontinence. There is an agreement that pelvic floor training must be a first-line treatment regime for stress and mixed urinary incontinence12. The pelvic floor muscle training is found to be more efficient if this regime is followed on a regular and intensive basis; also, the training must be acutely supervised and closely followed up by the trainer13. Although there is vital evidence in favor of pelvic floor training, there is still a growing interest among researchers to find alternative treatment regimens to treat stress urinary incontinence like the Pilates method, deep abdominal muscle training or Hypopressive exercises, Paula method, yoga training, and others. If it is being observed over the past many years that no significant advances have been made in the field of Physiotherapy for most of the diseases related to gynecological rehabilitation. But at the same time, some new theories have been proposed, and some latest modalities have been introduced in the clinics. Although patient care is being improved yet, there is a lack of evidence-based practice, especially in Asian countries like Pakistan. All of these techniques are being used worldwide but with a low level of evidence for their effectiveness10 .In Pakistan, due to a lack of awareness and resources, these techniques are not commonly in practice, and pelvic floor muscle training is the only reliable regime yet. But the currently available literature featuring these new therapies looks promising and may prove them as alternatives to pelvic floor muscle training. So, it is time to explore new prospects for gynecological rehabilitation in Pakistan so that every patient can get an enhanced quality of life. This short review aims to present all the latest available evidence regarding exercise-based physiotherapy techniques to treat stress urinary incontinence for females except Kegels exercises. According to author’s knowledge, there is no previous study being done on these specific techniques. This is important to mention that this study does not intend to compare the treatment strategies, still, it will provide currently available literature about the efficacy of these new therapies. So, physical therapists and clinicians will be able to propose a better treatment regime for urinary incontinence for their patients.
Methodology
The relevant studies and clinical trials were searched specifically investigating alternative exercise regimes like the Pilates method, deep abdominal muscle training or Hypopressive exercises, Paula method, and yoga training for adult females suffering from stress urinary incontinence. The electronic database; Google Scholar, the Cochrane Library, PubMed, Science Direct, and BMC journals were used for the literature search. The period for the literature search expanded from January 2022 to August 2022. In this review study, the randomized clinical trials were included if they were studying the Pilates method, deep abdominal muscle training or Hypopressive exercises, Paula method, and yoga training techniques other than Kegels. In this context, at least two latest available pieces of evidence were included regarding each treatment regime. While the trials investigating the pregnant, immediate post-partum females and females complaining of urge urinary incontinence were excluded. This is important to mention that this study does not intend to compare the treatment strategies, still, it will provide currently available literature about the efficacy of these new therapies. All the included studies are also presented in tabulated form so that it will be easy for the reader to extract the information. The treatment regimens that are included in this review are now shortly described here under these headings to understand their contextual facts and mechanism of action.
Exercise-Based Techniques:
Pilates Method:
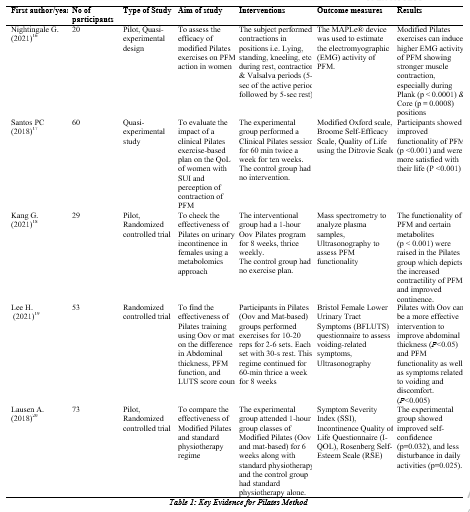
Joseph Pilates was a German physical trainer who invented the Pilates exercise program. In his early life, he suffered from multiple diseases that resulted in muscular weaknesses. So, he took it as a challenge and dedicated his life to becoming physically stronger and promoting this idea of fitness. He introduced this ideology of Pilates for physical and mental fitness and named this technique “Contrology”. The concept of Pilates is about coordinating body and mind through controlled movements. This program relies on eight principles; control, accuracy, breathing, awareness, isolation, centering, movement, and routine. The recommended Pilates exercises plan emphasizes breathing and the stimulation of the deep stabilizers of the trunk that is completely synchronizing with the pelvic floor muscles (PFM)14. It is said that Pilates plays a pivotal role in the enhancement of the “POWER HOUSE” of the body, which is considered as the abdomen, back, and PFM. In recent years, Pilates has become popular as a technique to attain strength, flexibility, and mind-body wellness and awareness15. Due to the increasing interest in this novel approach, there is a need for a scientific context for its application in regular clinical practice. A study conducted by Nightingale et al. (2020) concluded that pelvic floor muscles demonstrate a higher level of electromyographic activity (EMG) when held in modified Pilates positions16. A quasi-experimental trial was carried out to investigate the effect of clinical Pilates on the quality of life of older women in Portugal. It was concluded that clinical Pilates sessions held in the form of classes had a better impact on their self-efficacy and health condition17. Another fascinating study was conducted on Korean females, which technically verified the clinical benefits of Pilates. The researchers used a novel scientific method called Metabolomics. This is a comprehensive study of metabolical changes that occurred at the cellular level with physical activities such as Pilates. They assigned 29 subjects into three groups, UI group with Pilates (UIP, n=13), UI group with no Pilates (UINP, n=8), and control group (Control, n=8), respectively. The experiment was performed for eight weeks, and plasma samples were taken pre-and post-intervention; also ultrasonography was performed to evaluate the functional changes in pelvic floor musculature. The authors concluded that this novel approach can facilitate the practical outcome of PFM as well as the enhancement of metabolic features of these muscles. 18 In recent research articles, various approaches to performing Pilates were compared to know which maneuver is more effective for treating SUI. A clinical trial exhibited by Lee et al. (2021) compared two methods of Pilates; one was Oov-based Pilates, and the other was mat-based Pilates along with the symptomatic control group. The outcome parameters were the functional movement of PFM, the thickness of abdominal muscles, and the clinical score of lower urinary tract symptoms (LUTS). The study concluded that Oov-based Pilates was superior to the other regimes in terms of quantitative quality of abdominal muscle thickness and functional mobility of pelvic floor muscles. These parameters show that the severity of symptoms related to UI, like voiding and discomfort, was reduced19. Another pilot study compared the efficacy of Pilates and the standard physiotherapy approach. This study used a more holistic approach to Pilates called modified Pilates (MP) because urinary incontinence is not only limited to physical symptoms but also affects the social and mental capacity of the affected person. Seventy-three patients were randomly assigned to an interventional (Modified Pilates) group and a control (standard Physiotherapy) group. The participants were assessed based on their quality of life, confidence, and self-reporting of urinary incontinence. Post-intervention analysis showed that the MP group manifested a wide range of benefits including, better self-esteem, improved quality of life, and decreased disconcert. This study also proposed the feasibility of a large-scale randomized clinical trial20.
Deep Abdominal Hypopressive Training:
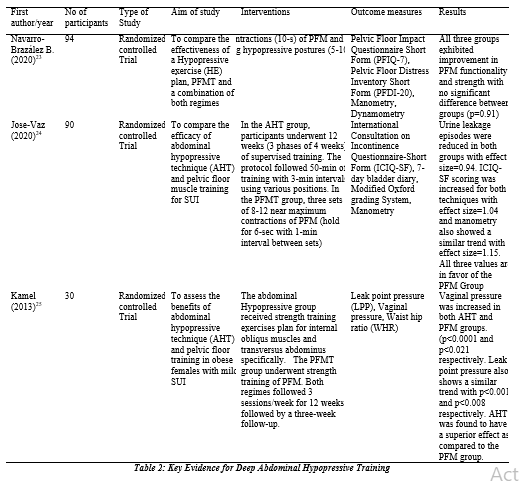
Contraction of deep abdominal muscles may help to co-contract the pelvic floor musculature. This hypothesis leads to the ideology that combined contraction of the pelvic muscles and deep abdominals may be more effective than specific pelvic floor training to enhance continence. In a study, conducted by Ghroubi et al., this hypothesis was affirmed in a trial which concluded that the pelvic floor and abdominals work synergistically, and there is a positive correlation between them. It was also concluded through these findings that SUI cannot be attributed entirely too pelvic floor weakness but abdominals also play their role21. This phenomenon was further emphasized by the results of another trial that concluded that abdominal muscle rehabilitation could be beneficial for the training of pelvic floor musculature22. A recent prospective study was conducted to compare the efficacy of Hypopressive exercises (HE) and pelvic floor muscle training, which is considered the gold standard for treating pelvic floor dysfunction (PFD). It was a parallel-group clinical trial with a 3-armed structure. The female subjects (n=94) with PFD were recruited for Hypopressive exercises (n=31), PFMT (n=32) and both (n=31). The study concluded that all the groups showed significant improvements from baseline data. None of the groups was superior to the other, and all three interventions reduced the PFD symptoms and improved the quality of life. And this improvement lasted both in the short and long term23. A single-blinded randomized trial was performed on symptomatic females with SUI to compare abdominal hypopressive and pelvic floor training. According to the post-intervention analysis, both groups showed improvements in the function of PFM and quality of life. However, the statistical values were more in favor of the pelvic floor training group when all the outcome measures were collectively observed24 . In another study, Kamel et al. (2013) conducted a study that compared abdominal and pelvic floor training to treat mild SUI. In this study, a total of thirty obese females with mild SUI were randomly allocated to 2 groups: the pelvic floor exercise (PF) group and the abdominal exercise (ABD) group. This study revealed that 12 weeks of specified abdominal training followed by improvised leak point and vaginal pressure, was superior over PFMT25.
Paula Method:
Paula Garbourg (1907-2004), the developer of the Paula method or ring muscle method, was born in Germany. At the age of 35, an illness confined her to a wheelchair. This disability encouraged her to decide that she would not give up on the situation. She devised and practiced this method on her own body, and she started to recover from that sickness and disability. Later on, it was proved effective through clinical trials in many orthopedic issues. The working theory behind the Paula method is that all the sphincters of the body act synchronously. While training the ring musculature of the mouth, eyes, or nose, will result in improving the strength and co-contraction of pelvic floor musculature26.
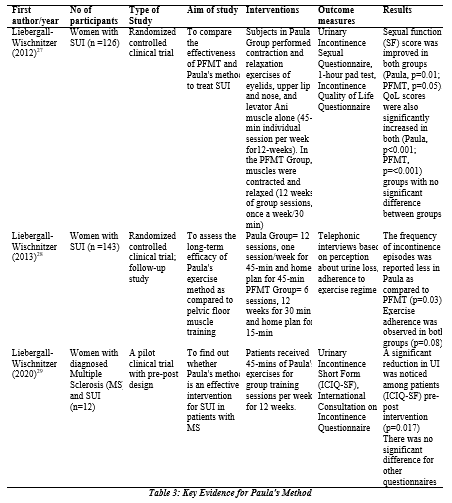
Among the clinical trials, one was performed by Liebergall-Wischnitzer in Israel, which evaluated the efficacy of the Paula method for stress incontinence and observed its effects on sexual functions and quality of life. The intervention consisted of 2 exercise regimens, i.e. the Paula method performed for 12 weeks and PFMT for 12 weeks of group sessions once a week, for four weeks. This RCT demonstrated that both the interventions manifested improvement of all outcome measures, no significant difference was found between groups27. The follow-up study for the same trial was done six months later to estimate the long-term effectiveness of the Paula method. There was no significant deterioration in SUI symptoms; in fact, the Paula group achieved a lower frequency of urinary leakage episodes than PFMT. However, the authors recommended the clarification of exercise regime duration and the generalization of exercise programs for females 28.
Another study further supported the efficacy of these circular muscle exercises for the treatment of UI in female patients of Multiple sclerosis. A total of 12 participants completed this pilot clinical trial and demonstrated a significant reduction in the ICIQ-SF score as a post-intervention result. However, regarding sexual functionality and quality of life (QoL), there were no significant changes before and after the intervention29 (Table 3).
Discussion
Stress urinary incontinence is a prevailing condition among females all over the world that has a massive impact on their social, emotional, economic, and physical aspects of life. Although various treatment options are available for urinary incontinence, still it is imperative to know which of them is considered a Gold standard. The most effective and safest treatment option is pelvic floor muscle training as per the clinical trials and evidence. Dumoulin et al. indicated in their study that PFMT has grade-A-level evidence of its effectiveness, and there is mutual consensus that pelvic floor training should be the first-line treatment method for mixed and stress UI30. Despite the strong evidence of its efficacy, authors are still struggling to treasure more novel approaches to treat urinary incontinence. In this context, the present study is a short appraisal of currently available evidence for the latest therapies for females diagnosed with SUI. The exercise-based approaches included in this study are Pilates, Deep abdominal training, and the Paula method. The author tried to present an overview of some new therapies to acknowledge the latest available literature, still, this study does not intend to make comparisons or critical appreciation to any of the studies included. All the trials describe each approach that is included in this study, whether this technique is effective or not according to the newest presented evidence. However, there is a model which demonstrates that novel interventions are not usually practiced in clinics unless these have been proven as an efficient approach in randomized clinical trials. It will stifle ideas, innovation, and further developmental progress31. With this background, a systematic review was presented in which they provided an agenda of how novel therapies are being included in regular clinical practice. They constructed a three-phased protocol which included the phases of development, testing, and dissemination or refinement32 . In the same perspective, Bo, Kari, et al. evaluated many new therapies according to this 3-phase protocol, which treatment technique falls in which phase. They concluded that breathing exercises, yoga, Tai Chi, posture correction, and fitness coaching are still in the developmental stage. So, according to their observation, there were not sufficient suggestions in support of strong evidence that alternative exercise programs can also play a role in the reduction of urinary leakage in women with SUI. As a conclusive statement, alternative exercise protocols should not still be recommended as a joint clinical practice for treating women diagnosed with SUI.
Conclusion
In conclusion, this study presents the ideology of inclusion of novel therapy approaches into regular clinical practice based on their latest literature-based evidence. All the approaches like Pilates, Paula, and Hypopressive training have been shown to have a positive impact on the treatment of stress urinary incontinence. No one technique was found to be completely ineffective; however, the range of usefulness may vary. There is also a necessity to conduct more trials as many methods are not repetitively tested under clinical trials. A minimal number of studies are available for techniques like Paula, the Yoga method, or many other interventions. So, we need to expand the clinical trial dimensions so that we can come out with better treatment options that will be equally beneficial for the patient and the clinician.
AUTHORS’ CONTRIBUTION:
The following authors have made substantial contributions to the manuscript as under:
Conception or Design: Sameera Mushtaq
Acquisition, Analysis or Interpretation of Data: Sameera Mushtaq
Manuscript Writing & Approval: Sameera Mushtaq, Dr. Ashfaq Ahmed
All authors acknowledge their accountability for all facets of the research, ensuring that any concerns regarding the accuracy or integrity of the work are duly investigated and resolved.
ACKNOWLEDGEMENTS: I thanks all the participants in this study.
INFORMED CONSENT: N/A
CONFLICT OF INTEREST: N/A
FUNDING STATEMENTS: N/A
ETHICS STATEMENTS: N/A
References
- Abufaraj M, Xu T, Cao C, Siyam A, Isleem U, Massad A, Soria F, Shariat SF, Sutcliffe S, Yang L. Prevalence and trends in urinary incontinence among women in the United States, 2005–2018. American journal of obstetrics and gynecology 2021;225(2):166-e1.
- Przydacz M, Chlosta M, Chlosta P. Population-Level Prevalence, Bother, and Treatment Behavior for Urinary Incontinence in an Eastern European Country: Findings from the LUTS POLAND Study. J. Clin. Med 2021;10(11):2314.
- Zhang RQ, Xia MC, Cui F, Chen JW, Bian XD, Xie HJ, Shuang WB. Epidemiological survey of adult female stress urinary incontinence. BMC Womens Health 2021;21:1-0.
- Hammad FT. Prevalence, social impact and help-seeking behavior among women with urinary incontinence in the Gulf countries: A systematic review. Eur J Obstet Gynecol Reprod Biol 2021; 266:150-6.
- AlQuaiz AM, Kazi A, AlYousefi N, Alwatban L, AlHabib Y, Turkistani I. Urinary Incontinence Affects the Quality of Life and Increases Psychological Distress and Low Self-Esteem. Healthc 2023 Jun 15 (Vol. 11, No. 12, p. 1772). MDPI.
- Hassan S, Malik KK, Khursheed MA, Seikh AH, Ali A, Siddiqui AA. Frequency of Different Types of Urinary Incontinence and Their impact on Quality of Life of Pakistani Women: Different Types of Urinary Incontinence and Their impact on Quality of Life. Pak BioMed J 2022:291-5.
- Pizzol D, Demurtas J, Celotto S, Maggi S, Smith L, Angiolelli G, et al. Urinary incontinence and quality of life: a systematic review and meta-analysis. Aging Clin Exp Res. 2021;33(1):25-35.
- Frawley H, Shelly B, Morin M, Bernard S, Bø K, Digesu GA, et al. An International Continence Society (ICS) report on the terminology for pelvic floor muscle assessment. Neurourol Urodyn. 2021;40(5):1217-60.
- Falah-Hassani K, Reeves J, Shiri R, Hickling D, McLean L. The pathophysiology of stress urinary incontinence: a systematic review and meta-analysis. Int Urogynecol J 2021; 32:501-52.
- Bø K, Herbert RD. There is not yet strong evidence that exercise regimens other than pelvic floor muscle training can reduce stress urinary incontinence in women: a systematic review. J Physiother. 2013;59(3):159-68.
- Wu JM. Stress incontinence in women. N Engl J Med. 2021 Jun 24;384(25):2428-36.
- Dumoulin C, Hay-Smith J. Pelvic floor muscle training versus no treatment for urinary incontinence in women. A Cochrane systematic review. Eur J Phys Rehabil Med. 2008;44(1):47-63.
- Bø K. Pelvic floor muscle training in the treatment of female stress urinary incontinence, pelvic organ prolapse and sexual dysfunction. World J Urol. 2012;30(4):437-43.
- Garcia-Falgueras A. An introduction to proprioception concept in pilates and yoga. Br J Med Med Res 2016;15(3).
- Muscolino JE, Cipriani S. Pilates, and the “powerhouse”—II. J Bodyw Mov Ther 2004;8(2):122-30.
- Nightingale G, Chandrakumaran K, Phillips C. The effect of modified Pilates-based positions on pelvic floor electromyographic (EMG) activity; a pilot study. Int Urogynecol J 2021;32(2):287-92.
- Santos PC, Lopes S, Teixiera RJ, Macedo C, Azevedo R, Mesquita C. Impact of clinical pilates on satisfaction with life of women with urinary incontinence. Advances in Mental Health Studies 2018:1-23
- Kang G, Lee H, Shin M, Kim J, Lee S, Park Y. The efficacy of Pilates on urinary incontinence in Korean women: a metabolomics approach. Metabolites 2021;11(2):118.
- Lee H, Kang G, Moon H, Lee J, Kang M, Kim M-K. The interventional benefit of Pilates using Oov and mat on middle-aged women with lower urinary tract symptoms: emphasis on abdominal muscle thickness and muscular function. J Exerc Rehabil 2021;17(3):192.
- Lausen A, Marsland L, Head S, Jackson J, Lausen B. Modified Pilates as an adjunct to standard physiotherapy care for urinary incontinence: a mixed methods pilot for a randomized controlled trial. BMC Womens Health 2018;18(1):1-12.
- Ghroubi S, Jelassi O, Abidi S, Trabelsi E, Ayed HB, Chlif M, et al. Association between isokinetic abdominal muscle strength, pelvic floor muscle strength and stress urinary incontinence severity. Prog Urol 2022;32(11):727-34.
- Sapsford RR, Hodges PW. Contraction of the pelvic floor muscles during abdominal manoeuvres. Arch Rehabil Res Clin Transl 2001;82(8):1081-8.
- Navarro-Brazález B, Prieto-Gómez V, Prieto-Merino D, Sánchez-Sánchez B, McLean L, Torres-Lacomba M. Effectiveness of hypopressive exercises in women with pelvic floor dysfunction: a randomised controlled trial. J clin med 2020;9(4):1149.
- Jose‐Vaz LA, Andrade CL, Cardoso LC, Bernardes BT, Pereira‐Baldon VS, Resende APM. Can abdominal hypropressive technique improve stress urinary incontinence? an assessor‐blinded randomized controlled trial. Neurourol Urodyn 2020;39(8):2314-21.
- Kamel DM, Thabet AA, Tantawy SA, Radwan MM. Effect of abdominal versus pelvic floor muscle exercises in obese Egyptian women with mild stress urinary incontinence: A randomised controlled trial. Hong Kong Physiother J 2013;31(1):12-8.
- Liebergall-Wischnitzer M, Hochner-Celnikier D, Lavy Y, Manor O, Arbel R, Paltiel O. Paula method of circular muscle exercises for urinary stress incontinence—a clinical trial. Int Urogynecol J 2005;16(5):345-51.
- Liebergall-Wischnitzer M, Paltiel O, Celnikier DH, Lavy Y, Manor O, Wruble ACW. Sexual function and quality of life of women with stress urinary incontinence: a randomized controlled trial comparing the Paula method (circular muscle exercises) to pelvic floor muscle training (PFMT) exercises. J Sex Med 2012;9(6):1613-23.
- Liebergall-Wischnitzer M, Paltiel O, Lavy Y, Shveiky D, Manor O, Hochner-Celnikier D. Long-term efficacy of Paula method as compared with pelvic floor muscle training for stress urinary incontinence in women: a 6-month follow-up. J ET Nurs 2013;40(1):90-6.
- Liebergall-Wischnitzer M, Shvieky D, Lavy Y, Noble A, Vaknin A. Paula Method (Circular Muscle Exercise) for Urinary Incontinence Symptoms of Women with Multiple Sclerosis: A Pilot Study. Int J Complement Altern Med (New York, NY). 2020;26(7):652-3.
- Hay‐Smith J, Dumoulin C. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women. Cochrane Database of Systematic Reviews 2006(1).
- Crosbie J. Does a stubborn commitment to ‘evidence’stifle innovative thinking? J Physiother 2013;59(2):69-71.
- Bø K, Herbert RD. When and how should new therapies become routine clinical practice? Physiotherapy 2009;95(1):51-7.
The Ziauddin University is on the list of I4OA, I4OC, and JISC.
This is an open- access article distributed under the terms of the Creative Commons Attribution License (CC BY 4.0).
