Hafsa Zahid1, Ayesha Jamil2*, Fariha Khalid3
1Master of Neurological Physical Therapy, The University of Lahore, Lahore, Pakistan![]()
2*Master of Philosophy in Physical Therapy, Lahore, Pakistan![]()
3Master of Neurological Physical Therapy, The University of Lahore, Lahore, Pakistan![]()
ABSTRACT
Background of the Study: To compare the effects of relaxing music therapy with task-oriented training of lower limbs on the balance and functional status in patients with chronic stroke.
Methodology: This randomized clinical trial was conducted in three outpatient physiotherapy clinics in Lahore, Pakistan. A sample of 76 participants with chronic stroke, aged 40-60 years, and on assistance walking, were recruited through a purposive sampling technique. Individuals who had physical impairments and visual or hearing deficits were not included in the study. Group A received task-oriented training with routine physical therapy while Group B received Music therapy additionally. Three sessions on alternate days per week for eight weeks were given. Balance and functional independence were the outcome variables measured using the Berg Balance Scale and Functional Independence Measure respectively. Mann-Whitney U test and Friedman ANOVA were applied for between-group and within-group differences respectively. P-value was significant at ≤0.05.
Results: The mean age of participants was 54.05 ± 3.64 years, the majority i.e., 55 (72.4%) were male, 46 (60.5%) had ischemic stroke and 53 (69.7%) were presented with left-sided weakness. A statistically significant difference was observed among both groups in balance (p =.000) and functional independence (p=0.000). The within-group difference was also significant for balance (p=0.000) and functional independence (p=0.000).
Conclusion: The integration of relaxing music therapy, task-oriented training, and routine physiotherapy is effective in improving balance and functional independence in chronic stroke patients.
Keywords: Balance, berg balance scale, functional independence, functional independence measure, music therapy, coordination impairment.

Introduction
Stroke or cerebrovascular accident (CVA) is the second leading cause of disability and mortality worldwide1. According to WHO, it can be interpreted as the quick development of impairments due to focal cerebral dysfunction that makes the patient’s life susceptible to secondary complications2. According to a survey in the USA, of 795,000 new sufferers of stroke around 26% live their life as a disabled person while hemi paresis leads to decreased mobility in about 50% of individuals3.Stroke is rated as the highest cause of disability in China, as over two million cases of stroke are reported every year4. In Turkey, the prevalence of stroke is 4.12% at ages over 44 years5. In Pakistan, the incidence of stroke is reported as 95 per 100,000 individuals annually from the year 2000 to 2016. The highest incidence is among the age group from 75-80 years6 with a 4.8% stroke survivors rate reported7. Stroke patients have cognitive, sensory, and motor impairments that cause difficulty in performing daily life activities. Cognitive complications create trouble in day-to-day tasks, problem-solving, and memory. Motor impairments include motor hindrances and functional impedances, in which deficiency in motor execution and learning with loss of versatility and balance is seen. Whereas, sensory limitations result in loss of proprioception and tactile stimulation8. Among the types of stroke, hemiplegia is the main motor demonstration of stroke which is described as weakness of one side of the body, opposite to the side of brain damage9. The recovery of functions after stroke takes place in three stages. Each stage has a unique set of neuromuscular disability10,11. The chronic stage is the last or third stage that starts after six months of onset and may stay with the individual for the rest of their life11. Many techniques are helpful in the recovery of stroke patients. Some techniques include CIMT, PNF techniques, Bobath therapy, stretching exercises, motor relearning programs, Rood’s therapy, ROM exercises, functional therapies, and strengthening exercises are used for the recovery of stroke patients and functional improvement of limbs12. Music therapy (MT) is an organized procedure of intervention using music as a background environment. It helps to improve the quality of life and promote emotional, physical, and social health by affecting the rhythm of respiration, reducing the stiffness of muscles, and decreasing blood pressure and heart rate. It also makes the environment comfortable and relieves the tension due to the increased alpha waves in the brain13. Music therapy utilizes two modes; in the active process, the client plays a role in the creation of music while in the passive process, he/she responds or listens to music14. Different techniques are used in music therapy such as Musical Neglect Training, Rhythmic Auditory Stimulation, and Therapeutic instrumental Musical Performance to integrate the movement in an individual15. Task-oriented training is directed at improving control strategy, to minimize inappropriate movements. It eases the functional status of neuromusculoskeletal systems16. For the lower extremity, it includes bicycling, circuit and treadmill training, sit-to-stand exercises, reaching tasks, and walking training on the ground to improve balance while upper extremity training includes CIMT, mental imagery, and grasping objects17. The combination of relaxing music intervention with task-oriented training on lower limb functions in stroke patients is not yet identified. Therefore, this study aims to find out the combined effects of these therapies to gain advancement in balance and functional independence in chronic stroke patients.
Methodology
This study was designed according to the guidelines of Consolidated Standards of Reporting Trials (CONSORT). This randomized clinical trial was registered in ClinicalTrial.gov with ID: NCT05446207. Ethical approval to conduct this study was taken from the Research Ethical Committee of The University of Lahore, (Ref Id: REC-UOL-/147-06/2022) and conducted according to the guidelines of Helsinki. Informed consent was provided by the participants. The objectives of the study were explained to them. Confidentiality was ensured. The anonymity of the participants and the right to withdraw were also reserved.
This study was conducted from June 2022 to December 2022 at three outpatient physiotherapy departments of The University of Lahore Teaching Hospital, Social Security Teaching Hospital, and Yaseen Medical Centre, Lahore, Punjab, Pakistan. A sample of 76 patients (38 in each group), calculated through OpenEpi software using a mean score of Berg Balance Scale (BBS) 18, 95% level of significance, and 80% power of the study, were selected using a purposive sampling technique. Both male and female of age 40-60 years, with chronic CVA diagnosed by neuro physician within 6 months of onset disease and BBS score ≥ 20 ≤ 40 and Functional Independence Measure (FIM) score up to 3 (needs moderate assistance) and able to understand the command, Mini-Mental State Examination (MMSE) score of over 20 were included in the study. Any participant having systematic disorders such as rheumatoid arthritis, unstable angina, and coexisting physical impairments e.g., limb amputation, previous history of fractures, any neurological disease other than stroke, and visual or hearing deficits were excluded from the study.
Three physiotherapists with an average experience of five years in dealing with neurological conditions were involved in the study. Opaque, transparent sealed envelopes were used to divide the participants into two groups. Group A received routine physiotherapy treatment along with task-oriented training of the lower extremity. Routine physiotherapy included hot packs, stretching, and strengthening exercises. Walking, sit-to-stand, leg curling, an extension of the leg, pressing of the leg, and reaching tasks e.g., grasping of objects, dynamic balance, etc. were included in task-oriented training. Around two sets of 10 repetitions of each activity, with a rest period of two to three minutes between each set of training were performed. Group B received passive relaxing music therapy in addition to routine physiotherapy and task-oriented training for the lower limbs. A relaxing music of the same tone and frequency was provided for 15 min to all patients through headphones having voice cancellation properties. The total duration of each session was 45 minutes. Treatment was given for three days on an alternative basis per week up to eight weeks. Balance was assessed using the Berg Balance Scale (BBS) while functional independence was calculated through the Functional Independence Measure (FIM). Outcome variables were recorded at baseline, in the 4th and 8th weeks by an independent accessor, who was unaware of the treatment group. The entire process of patient screening to allocation till follow-up is represented in Figure # 1.The data was analyzed using the latest version of SPSS (Version-24). The data in numerical form as age, BBS score, and FIM score were formulated in mean ± SD. The data of categorical variables was given in the form of frequency or percentage. The data normality was observed using the Kolmogorov-Smirnov test (p< 0.05). The assumptions of normality were not met, so non-parametric tests were used to measure the between-group and within-group differences. The differences between the two groups regarding balance and functional independence were calculated by using the Mann-Whitney U Test. Friedman ANOVA was used for within-group comparison of score of balance and functional independence at baseline, 4th week, and 8th week. The median ± Inter Quartile Range was the measure used for the expression of balance and functional independence score. Intention to treat (ITT) analysis was used to manage missing data on lost to follow-up participants. A P-value less than 0.05 was considered significant.
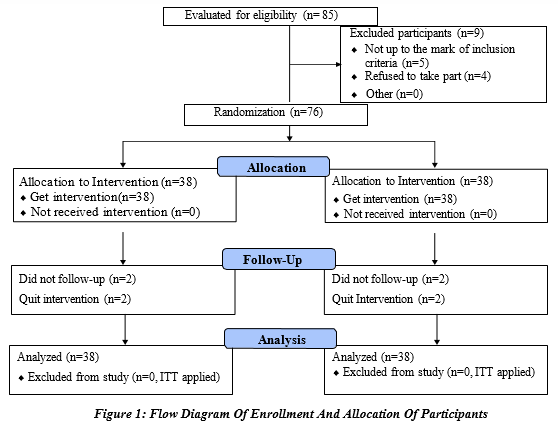
Results
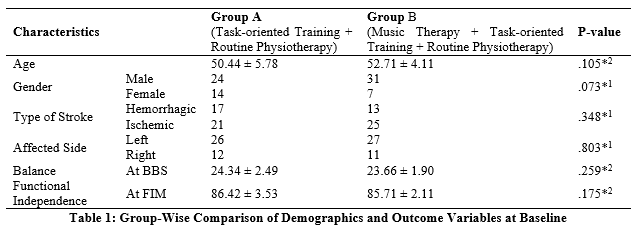
The mean age of the participants was 54.05 ± 3.64 years. Among 76 participants, 55 (72.4%) were male and 21 (27.6%) were females. Around 46 (60.5%) participants had an ischemic stroke while 30 (39.5%) had a hemorrhagic stroke, 53 (69.7%) presented with left-side weakness, and 23 (30.3%) presented with right-side weakness. The results of group-wise comparison given in Table # 1 indicated that the participants in groups A and B were the same based on demographic characteristics and outcome measurements at baseline (p> 0.05).
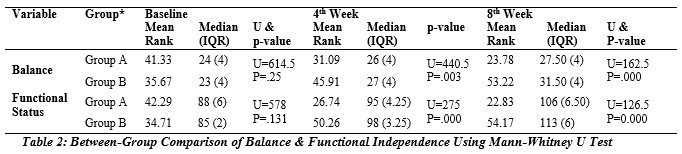
P-value was calculated using chi-square analysis*1 and independent sample-t-test*2. Table # 2 shows the mean ranks and median (interquartile range) of both groups and it represents that the balance score was statistically significantly higher in group B than in group A in the 8th week (U=162.5, p=.000). Moreover, the functional independence was improved significantly in group B than group A (U=126.5, p=0.000).
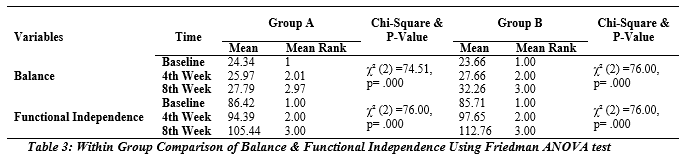
*The total number of participants in both group were 38 from baseline till the 8th week. Table # 3 reveals that there was a statistically significant improvement in balance and functional independence of groups A and B from baseline (p=0.000) till the 8th week (p=0.000).
Discussion
A significant improvement in balance and functional independence with the incorporation of music therapy along with task-oriented training and routine physical therapy was seen in this study. It is concluded that music therapy can play a promising role in addressing gross motor impairments of the lower extremities in patients with stroke. A study was conducted by Park J-S et.al to find the effects of core muscle stability exercises about music therapy on balance and functional activity in stroke patients. The experimental group received music therapy with core stability exercises five times a week. Treatment was given for eight weeks19. Improvement in gait, walking ability, and functional independence was also observed in a quasi-experimental study by Samira, et al., using music-based rhythmic auditory stimulation (RAS) in combination with physical therapy in stroke patients at the sub-acute stage20. A similar clinical study by Wang et al., on ischemic stroke patients resulted in the benefits of music therapy on walking ability, balance and gait, and overall lower extremity function. Music therapy was given for six days a week for up to one month21. A systematic review conducted by Daniel et al., in 2021 also supports music therapy and its effectiveness on the gait after stroke22. A systematic review was conducted by Le Perf et al., to identify the effectiveness of music therapy and its types in the rehabilitation of stroke. They concluded in their review that gait parameters and balance have a positive effect on music therapy. They included twenty-seven studies in their review23. A case study was done by Ronning J and Smith C in which they checked the combined effects of physical therapy and music therapy on a stroke patient. The patient received 11 one-hour sessions for 11 weeks. Multiple interventions were implied including gait training with RAS, TIMP, and PNF techniques. When the patients were reassessed, the score on the Berg Balance Scale was increased24.
Conclusion
Likewise, Fotakopoulos, G. and Kotlia, P. concluded that the addition of music to exercise programs in the rehabilitation of stroke patients provides a better improvement in cognition, muscle strength, and motor abilities of the affected side with the provision of music therapy daily up to six months compared to the current study in which music therapy was given on alternate days up to eight weeks25. Music therapy was also observed to improve the motor function of the upper limb as depicted by the study of Tong et al.,25 in which effects of supported music therapy were seen to improve the upper limb motor functions in post-stroke patients. They took two groups one group was an audible music group while the other one was a mute music group. In our study, we differentiated with the addition of task-oriented training, and the study was mainly focused on lower limbs. In parallel to the findings of the current study, a pilot study organized by Cha et al., in 2014 documented the effects of rhythmic auditory stimulation with intensive gait training. Their results showed that control in posture and gait was improved in chronic stroke patients by incorporating music therapy for six weeks. They provided auditory stimulation via cue-based digital instruments contrary to our study used noise cancellation headphones with relaxing music26. The addition of music therapy is proven to be beneficial for chronic stroke patients. It can help improve the balance and functional independence of patients. This study’s findings can assist physical therapists in reducing disability and enhancing the quality of life for stroke patients. The outcome measure tools were subjective.
AUTHORS’ CONTRIBUTION:
The following authors have made substantial contributions to the manuscript as under:
Conception or Design: Hafsa Zahid, Ayesha Jamil, Fariha Khalid
Acquisition, Analysis or Interpretation of Data: Ayesha Jamil, Hafsa Zahid
Manuscript Writing & Approval: Ayesha Jamil, Hafsa Zahid, Fariha Khalid
All authors acknowledge their accountability for all facets of the research, ensuring that any concerns regarding the accuracy or integrity of the work are duly investigated and resolved.
ACKNOWLEDGEMENTS: we would like to express our deepest gratitude to our colleagues, hospital staff, and attendants of patients for their cooperation in this study.
INFORMED CONSENT: Informed consent was taken from all the study participants.
CONFLICT OF INTEREST: NIL
FUNDING STATEMENTS: The authors received no financial support for the research.
ETHICS STATEMENTS: The protocol of the present study was registered by the Research Ethical Committee of The University of Lahore, approval code; REC-UOL-/147-06/2022)/registered in Clinical Trial.gov NCT05446207.
References
- Lindsay MP, Norrving B, Sacco RL, Brainin M, Hacke W, Martins S, et al. World Stroke Organization (WSO): Global Stroke Fact Sheet 2019. International Journal of Stroke. 2019;14(8):806-17. DOI: 10.1177/1747493019881353.
- Bae S-H, Kim T-G, Lee Y-S, Hwang J-A, Jeon B-H, Kim K-Y. The Effects of Median Nerve Mobilization Therapy on Stroke Patients with Carpal Tunnel Syndrome; A Pilot Study. International Information Institute (Tokyo) Information. 2018;21(2):831-42. Retrieved from https://www.proquest.com/openview/4d2d19686f84cbe5274706029c2c4d90/1?pq-origsite=gscholar&cbl=936334
- Katan M, Luft A, editors. Global burden of stroke. Seminars in neurology; 2018: Thieme Medical Publishers. DOI: 10.1055/s-0038-1649503.
- Wu S, Wu B, Liu M, Chen Z, Wang W, Anderson CS, et al. Stroke in China: Advances and challenges in epidemiology, prevention, and management. The Lancet Neurology. 2019;18(4):394-405. DOI: 10.1016/S1474-4422(18)30500-3.
- Padir Şensöz N, Türk Börü Ü, Bölük C, Bilgiç A, Öztop Çakmak Ö, Duman A, et al. Stroke epidemiology in Karabük city Turkey: Community-based study. eNeurologicalSci. 2018;10:12-5. DOI: 10.1016/j.ensci.2017.12.003.
- Khan MI, Khan JI, Ahmed SI, Ali S. The epidemiology of stroke in a developing country (Pakistan). Pakistan Journal of Neurological Sciences (PJNS). 2019;13(3):30-44. Retrieved from https://ecommons.aku.edu/pjns/vol13/iss3/9
- Singh V, Dhamoon MS, Alladi S. Stroke risk and vascular dementia in South Asians. Current atherosclerosis reports. 2018;20(9):1-7. DOI: 10.1007/s11883-018-0745-7.
- Xu C, He Z, Shen Z, Huang F. Potential benefits of music therapy on stroke rehabilitation. Oxidative Medicine and Cellular Longevity. 2022;2022. DOI: https://doi.org/10.1155/2022/9386095
- Guggisberg AG, Koch PJ, Hummel FC, Buetefisch CM. Brain networks and their relevance for stroke rehabilitation. Clinical Neurophysiology. 2019 Jul 1;130(7):1098-124. DOI: https://doi.org/10.1016/j.clinph.2019.04.004
- Sumakul VD, Notobroto HB, Widani NL, Aima MH. Instrumental music therapy reduced depression levels in stroke patients. Journal of Public Health Research. 2020 Jul 3;9(2):jphr-2020. DOI: https://doi.org/10.4081/jphr.2020.1847
- Miladinia M, Voss JG, Molavynejad S, Malehi AS, Zarea K, Nouri EM, Ahmadzadeh A. Slow-stroke back massage compared with music therapy for leukemia-related pain and fatigue: a randomized controlled trial. JCO Oncology Practice. 2021 Nov;17(11):e1614-21. DOI: 10.1200/OP.21.00156 JCO Oncology Practice17, no. 11 (November 01, 2021) e1614-e1621.
- Carlsson AM. Assessment of chronic pain. I. Aspects of the reliability and validity of the visual analog scale. Pain. 1983;16(1):87-101. DOI: 10.1016/0304-3959(83)90088-X.
- Wang S, Agius M. The use of music therapy in the treatment of mental illness and the enhancement of societal well-being. Psychiatria Danubina. 2018;30(Suppl 7):595-600. Retrieved fromhttps://www.psychiatriadanubina.com/UserDocsImages/pdf/dnb_vol30_noSuppl%207/dnb_vol30_noSuppl%207_595.pdf
- Šuriņa S, Duhovska J, Mārtinsone K. Music therapy for stroke patients: a systematic review with meta-analysis. InSOCIETY. INTEGRATION. EDUCATION. Proceedings of the International Scientific Conference 2019 May 21 (Vol. 4, pp. 287-300). DOI:http://dx.doi.org/10.17770/sie2019vol4.3860
- Leverington J, Bell K. Collaborative Physical and Music Therapy Interventions for Impairments of Chronic Stroke: A Case Study. 2019. Retrieved from https://commons.und.edu/cgi/viewcontent.cgi?article=1671&context=pt-grad
- Street A, Zhang J, Pethers S, Wiffen L, Bond K, Palmer H. Neurologic music therapy in multidisciplinary acute stroke rehabilitation: could it be feasible and helpful? Topics in stroke rehabilitation. 2020;27(7):541-52. DOI: https://doi.org/10.1080/10749357.2020.1729585
- Huang W-H, Dou Z-L, Jin H-M, Cui Y, Li X, Zeng Q. The effectiveness of music therapy on hand function in patients with stroke: A systematic review of randomized controlled trials. Frontiers in Neurology. 2021;12:641023. DOI: https://doi.org/10.3389/fneur.2021.641023
- Ruotsalainen J, Carlson E, Erkkilä J. Rhythmic exercises as tools for rehabilitation following cerebellar stroke: A case study integrating music therapy and physiotherapy techniques. Nordic Journal of Music Therapy. 2022 Oct 20;31(5):431-53. DOI: https://doi.org/10.1080/08098131.2022.2026452
- Park J-S, Yang K-H, Lee D-H. The Effects of Core Stability Exercise with Music on Balance and Functional Activity in Stroke. Journal of Korean Society for Neurotherapy. 2022;26(1):29-34. DOI: http:dx.doi.org/10.17817/2022.01.25.1111712
- Gonzalez-Hoelling S, Bertran-Noguer C, Reig-Garcia G, Suñer-Soler R. Effects of a music-based rhythmic auditory stimulation on gait and balance in subacute stroke. International journal of environmental research and public health. 2021;18(4):2032. DOI: 10.3390/ijerph18042032.
- Wang Y, Pan W-Y, Li F, Ge J-S, Zhang X, Luo X, et al. Effect of Rhythm of Music Therapy on Gait in Patients with Stroke. Journal of Stroke and Cerebrovascular Diseases. 2021;30(3):105544. DOI: 10.1016/j.jstrokecerebrovasdis.2020.105544. Epub 2020 Dec 17.
- Daniel A, Koumans H, Ganti L, Daniel AR. Impact of music therapy on gait after stroke. Cureus. 2021;13(10). DOI: 10.7759/cureus.18441
- Le Perf G, Donguy AL, Thebault G. Nuanced effects of music interventions on rehabilitation outcomes after stroke: a systematic review. Topics in Stroke Rehabilitation. 2019 Aug 18;26(6):473-84. DOI: https://doi.org/10.1080/10749357.2019.1623518
- Ronning, Jamie and Smith, Kayla, “Physical Therapy and Music Therapy Collaboration for the Treatment of Chronic Stroke: A Case Study” (2020). Physical Therapy Scholarly Projects. 691. https://commons.und.edu/pt-grad/691
- Fotakopoulos G, Kotlia P. The Value of Exercise Rehabilitation Program Accompanied by Experiential Music for Recovery of Cognitive and Motor Skills in Stroke Patients. Journal of stroke and cerebrovascular diseases: the official journal of National Stroke Association. 2018;27(11):2932-9. DOI: 10.1016/j.jstrokecerebrovasdis.2018.06.025. Epub 2018 Jul 30.
The Ziauddin University is on the list of I4OA, I4OC, and JISC.
This is an open- access article distributed under the terms of the Creative Commons Attribution License (CC BY 4.0).
