Tooba Jamil1, Hina Gul2*, Shoaib Waqas3, Roohi Abbas4
1House Officer Ghurki Trust Teaching Hospital (GTTH), Lahore, Pakistan![]()
2*Assistant Professor Lahore College of Physical therapy, LM&DC Lahore, Pakistan![]()
3Associate Professor Lahore College of Physical therapy, LM&DC Lahore, Pakistan![]()
4Assistant professor Lahore College of Physical therapy, LM&DC Lahore, Pakistan![]()
Abstract
Background and Aim: Headache is a very common condition worldwide. Cervicogenic headache is a secondary type of headache. Dentistry requires both, the concentration and precision and dentists have to work in constricted zones for extended period of time so it is important to evaluate headache among dental population. The objective of this study was to screen Cervicogenic headache among dentists working in Lahore Medical and Dental College, Lahore.
Methodology: The Descriptive Cross-sectional study, of 6 months duration, was conducted on 125 dentists. The data was collected from Lahore Medical and Dental College, Lahore. Non-Probability convenience sampling technique was used. Dentists working for at least 2 years and more than 5 hours daily, with the known cases of headache were included and those who were diagnosed with any other condition that cause headache like acute sinusitis, High blood pressure etc. were excluded. Data was collected by using cervical Flexion Rotation test whose validity is 0.81. Data was entered by using Statistical package for Social Sciences (SPSS) version 21 and the same software was used for data analysis.
Results: The findings showed that, out of 125 dentists, 36.8% (n=46) were male and 63.2% (n=79) were female and cervical flexion rotation test was positive in 30.4% (n=38) dentists.
Conclusion: This study concluded that cervicogenic headache is present in 30.4% dentists working in Lahore Medical and Dental College.
Keywords: Cervicogenic, occupational hazards, headache, musculoskeletal disorders, dentists, cervical pain.
Introduction
One of the significant public health issue is Headache1,2. It is the most frequent medical condition and the important reason for the utilization of medicines among general population3. Headaches are very much prevalent and have negative kind of effects on health4. These are basically of two categories, one is Primary and the other is Secondary. Those headaches are considered Primary which are of muscular (tension type) and vascular origin (migraine and cluster headache). Secondary headaches are those which occurs due to any other source like head and neck lesion or swelling5. One of the common Secondary headache is “Cervicogenic headache” which involves unilateral headache that refers from cervical spine or its components6. Of all kinds of headaches affecting global population, Cervicogenic headache accounts for 15-20% headaches with women affecting four times greater as compare to men7. According to recent studies, the pain in face and head in cervicogenic headache is usually due to cranial nerves(C1-C3) and also due to pathophysiological changes that occurs in cervical zygapophyseal joints (upper)8. Cervical pain and discomfort, as compare to distal regions like elbow and hand, also has a very high prevalence among dentists9.
Dental practitioners usually use to work in constricted zones for extended period of time in very uncomfortable positions which requires intemperate use of hands, back, neck and vision2. Dentistry is basically a very demanding profession which requires both, the concentration and precision. This profession is established on social interaction that is present between patients and care providers10. It is a distinctive job with concern to occupational hazards as well as the work demands.
A lot of importance has been given to ergonomics in dental profession in last few years and this is because of the increasing number of work related health problems in Dentist11. Health problems and dangers in dentistry can be categorized as psychological, physical, chemical, biomechanical and ergonomic12. According to the study conducted in Saudi Arabia, frequency of neck pain among Dentists is 66%13. Another study was done in 2006, which conclude that the persons with cervicogenic headache were having very low range of cervical extension/flexion14.
Malavde, Rutuja; Salunkhe, Pragati conducted research in 2020 on 81 middle aged dentists. The aim of the study was to check the presence of head ache among dental practitioners. They used observational study in which female gender was dominant. The outcome measures used were flexion rotation test and neck disability index. The conclusion of the study was 26.73% dental population suffered from cervicogenic headache16.
Another study conducted in 2018 on the prevalence of musculoskeletal problems among dentists. The aims of the study were to find the occurrence of musculoskeletal problems specifically neck, back and shoulder pain. The sample size of this research was 105 and an electronic questionnaire was used. This cross sectional study was conducted in Jeddah, Saudi Arabia. The results of this study showed that there was increased prevalence of musculoskeletal disorders in dentists18.
Another study conducted on 182 dental students in 2018. Dental students of first, third and final professional year were included in this study. This study aims to find out the occurrence of musculoskeletal disorders in dental students. A questionnaire was used to find the presence of musculoskeletal problems among participants. The results showed that girls were more susceptible to musculoskeletal disorders as compared to men. This study also showed that the most common site of musculoskeletal disorders is back and neck and these disorders are equally prevalent throughout the dental studies20.
A research conducted in 2016 on dental students of Naresuan University in Thailand. The study aims to find the frequency and risk factors related to musculoskeletal disorders in final year students of dentistry. The sample size was 68 and modified Nordic Musculoskeletal Questionnaire was used as a tool. The study concluded an increased incidence of neck pain due to poor posture and they suggest incorporating mild exercises in order to reduce the occurrence of musculoskeletal disorders21.
Arthisri, A S; Jain, Ashish R; Philip, Jacob Mathew; Krishnan et al conducted a research in 2017 on dental practitioners. The major aim of this study was to find the work related musculoskeletal disorders among dentists. The sample size was 297 dental practitioners and stratified sampling technique was used. According to this study the major sites affected due to dental profession were shoulder and low back. This study suggests to use proper ergonomic furniture and to perform regular workouts in the form of relaxation and postural exercises22.
A recent research conducted on the prevention of musculoskeletal disorders through ergonomic interventions in 2020. The main purpose of this study was to check the effect of proper ergonomics on the incidence of musculoskeletal problems in dental population. The research introduces multiple ergonomic design chairs and then follows up their effects on the prevention of musculoskeletal problems. This study proved a positive role of the ergonomic design furniture on the prevalence of musculoskeletal disorders in dentists23.
Rationale
To screen the Cervicogenic headache among dentists working in Lahore Medical and Dental College and to provide epidemiological data. This would be beneficial in providing awareness of the successful assessment and diagnosis of this type of headache.
Methodology
Study design
Descriptive Cross-sectional study.
Study duration
6 months duration after the approval of synopsis.
Sample size
125 dentists.
Study setting
Lahore Medical and Dental College, Lahore.
Sampling technique
Probability convenience sampling technique.
Inclusion criteria
Dentists working for at least 2 years and more than 5 hours daily, with the known cases of headache were included.
Exclusion criteria
Those who were diagnosed with any other condition that can cause headache were excluded.
Data collection tool
Data was collected by using Flexion Rotation test whose validity is 0.81. (14) This test is performed in supine lying. Examiner passively positions the patient’s neck into full flexion. Then head is passively rotated in each direction while flexed position is maintained. A prior consent of all the participants was taken.
Data analysis
The data was analyzed using SPSS version 25 and all variables are represented in form of frequencies and percentages. Results are presented in tables and figures.
Results
In 125 practitioners, 36.8% (n=46) were male and 63.2% (n=79) were female. As shown in the below table:

Table 1: Frequency of male and female
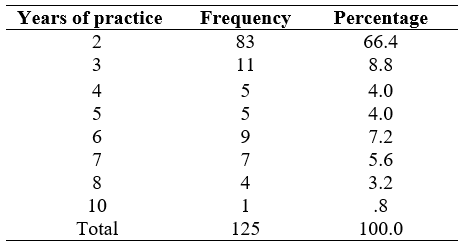
Table 2: Years of Practice
Out of 125 practitioners, 66.4%(n=83) were working for 2 years, 8.8%(n=11) were working for three years., 4%(n=5) were working for four years, 4%(n=5) were working for five years, 7.2% (n=9) were working for six years, 5.6% (n=7) were working for seven years, 3.2%(n=4) were working for eight years and 0.8% (n=1) were working for10 years.
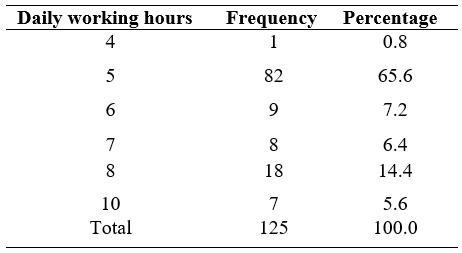
Table 3: Daily working hours
Out of 125 practitioners,0.8%(n=1) was working for 4 hours, 65.6%(n=82) were working for 5 hours, 7.2%(n=9) were working for 6 hours, 6.4%(n=8) were working for 7 hours, 14.4%(n=18) were working for 8 hours and 5.6%(n=7) were working for 10 hours.
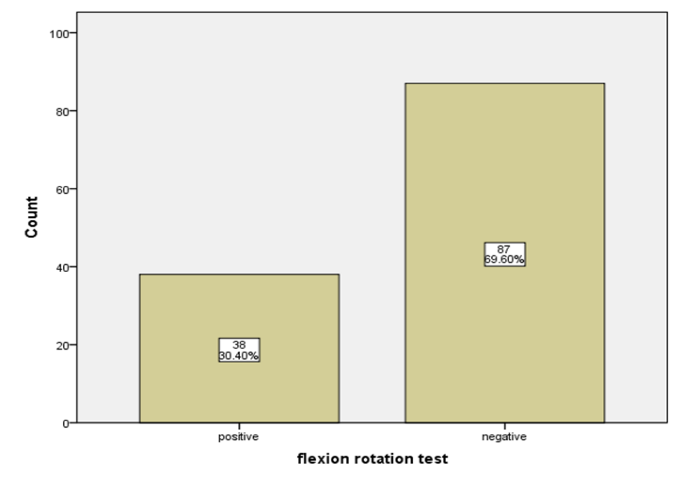
Figure 1: Bar graph showing results of cervical flexion rotation test
Flexion rotation test was positive in 30.4% (n=38) participants and negative in 69.6% (n=87) participants, out of total 125 dentists.
Outcome Measures
Cervical Flexion Rotation test.
Discussion
Headache is a most common condition worldwide15. The current study screened cervicogenic headache among dentists who have been working for at least two years to maximum ten years for more than 5 hours daily. For this purpose flexion-rotation test was used. Purpose of this screening was working posture of dentists, because it is often seen that a sustained posture for long duration adversely affects joints and muscles. This study concluded that cervicogenic headache was present among 30.4% dentists out of 125 and among those 36.8 %( n=46) were male and 63.2 %( n=79) were female.
A recent systematic review and meta-analysis is done by E. Anarte- Lazo et al in 2021. They conducted this research on the distinguishing features of migraine headache, cervicogenic headache and asymptomatic headache. The aim of this study was to differentiate between these three categories through symptoms and manual tests. For this purpose they use cervical flexion rotation test and manual muscle testing. This study proved that cervical flexion rotation test is a gold standard tool in order to diagnose cervicogenic headache24. So in the current study, cervical flexion rotation test was used which showed that cervicogenic headache was present among 30.4% dentists out of 125. It was seen that the reason behind this was due poor biomechanics24.
In 2014, Gokcen et al conducted a study on the importance of craniovertebral and cervico- medullary angles in cervicogenic headache on the patients with diagnosed cervicogenic headache and concluded that as their craniovertebral and cervico-medullary angles decreased their pain scores increased. Similarly, in current study those dentists who had poor biomechanics and bad posture, the craniovertebral and cervico-medullary angles decreased and in turn causes cervicogenic head ache22.
SamerNarouze MD in 2018, conducted a research on cervicogenic headache. The research revealed that cervicogenic headache is more evident in females as compared to men. The results of current study also show that cervicogenic headache is more prevalent in females as compared to men among dentists25. The reason behind this is that the bad posture is more common in females as compared to male.
Shimohata et al, in 2017, conducted a cross sectional study including 70 patients with cervical spine disorders who were scheduled to undergo fusion or laminoplasty. Preoperatively, headache was diagnosed among them and they concluded that cervicogenic headache was present in 15/70 and these patients also have high frequency of neck pain21. Similarly in the current study, cervicogenic headache was present in those dentists that have poor biomechanics.
Limitations of the study were small size due to limitation of time and non-cooperating participants regarding test position. Recommendation of the study is that the future study should be conducted on cervicogenic headache that should include complete assessment of Dentist’s posture and ergonomics etc. A comparative study should be conducted on Prevalence of cervicogenic headache among male and female.
Conclusion
This study concluded that cervicogenic headache was present among 30.4% dentists out of 125 and among those 36.8% (n=46) were male and 63.2% (n=79) were female.
AUTHORS’ CONTRIBUTION:
The following authors have made substantial contributions to the manuscript as under:
Conception or Design: Tooba Jamil
Acquisition, Analysis or Interpretation of Data: Hina Gul
Manuscript Writing & Approval: Shoaib Waqas, Roohi Abbas
All authors acknowledge their accountability for all facets of the research, ensuring that any concerns regarding the accuracy or integrity of the work are duly investigated and resolved.
ACKNOWLEDGEMENTS: We thanks all the participants in this study.
INFORMED CONSENT: Written Informed Consent was taken from each patient.
CONFLICT OF INTEREST: The author (s) have no conflict of interest regarding any of the activity perform by PJR.
FUNDING STATEMENTS: None declared
ETHICS STATEMENTS: The study has been approved by from the Ethics Committee of National hospital and medical center, DHA Lahore (Reference #NHMC/PT/021/2021
References
- Schramm S, Uluduz D, Gouveia RG, Jensen R, Siva A, Uygunoglu U, et al. Headache service quality: evaluation of quality indicators in 14 specialist-care centres. The journal of headache and pain. 2016;17(1):111.
- Al-Shehri Z, Al-Zoughool M. Self-reported musculoskeletal symptoms among dentists in Saudi Arabia. Industrial health. 2017:2016-0174.
- Jahani P, Salesi M, Marzban M, Abdollahifard G. The prevalence of headache among athletic university students.Asian journal of sports medicine. 2016;7(1).
- Pellesi L, Benemei S, Favoni V, Lupi C, Mampreso E, Negro A, et al. Quality indicators in headache care: an implementation study in six Italian specialist-care centres. The journal of headache and pain. 2017;18(1):55.
- Page P. Cervicogenic headaches: an evidence-led approach to clinical management. International journal of sports physical therapy. 2011;6(3):254.
- Chaibi A, Russell MB. Manual therapies for cervicogenic headache: a systematic review. The journal of headache and pain. 2012;13(5):351.
- Racicki S, Gerwin S, DiClaudio S, Reinmann S, Donaldson M. Conservative physical therapy management for the treatment of cervicogenic headache: a systematic review. Journal of manual & manipulative therapy. 2013;21(2):113-24.
- Xiao H, Peng B, Ma K, Huang D, Liu X, Lu Y, et al. The Chinese Association for the Study of Pain (CASP): Expert Consensus on the Cervicogenic Headache. Pain Research and Management. 2019;2019.
- Feng B, Liang Q, Wang Y, Andersen LL, Szeto G. Prevalence of work-related musculoskeletal symptoms of the neck and upper extremity among dentists in China. BMJ open. 2014;4(12):e006451.
- Hodacova L, Sustova Z, Cermakova E, Kapitan M, Smejkalova J. Self-reported risk factors related to the most frequent musculoskeletal complaints among Czech dentists. Industrial health. 2014:2013-0141.
- Ohlendorf D, Erbe C, Nowak J, Hauck I, Hermanns I, Ditchen D, et al. Constrained posture in dentistry–a kinematic analysis of dentists. BMC musculoskeletal disorders. 2017;18(1):291.
- Vodanović M, Sović S, Galić I. Occupational health problems among dentists in Croatia. ActastomatologicaCroatica. 2016;50(4):310.
- Aljanakh M, Shaikh S, Siddiqui AA, Al-Mansour M, Hassan SS. Prevalence of musculoskeletal disorders among dentists in the Ha’il Region of Saudi Arabia. Annals of Saudi medicine. 2015;35(6):456-61.
- Zito G, Jull G, Story I. Clinical tests of musculoskeletal dysfunction in the diagnosis of cervicogenic headache. Manual therapy. 2006;11(2):118-29.
- Krogh A-B, Larsson B, Salvesen Ø, Linde M. Assessment of headache characteristics in a general adolescent population: a comparison between retrospective interviews and prospective diary recordings. The journal of headache and pain. 2016;17(1):14.
- Malavde R, Salunkhe P. Prevalence of Cervicogenic Headache in Dentists. Indian Journal of Public Health Research & Development. 2020 May 1;11(5).
- Stovner LJ, Al Jumah M, Birbeck GL, Gururaj G, Jensen R, Katsarava Z, et al. The methodology of population surveys of headache prevalence, burden and cost: Principles and recommendations from the Global Campaign against Headache. The journal of headache and pain. 2014;15(1):5.
- Alogaibi YA, Alhowaish MA, Baokbah RA. Prevalence of musculoskeletal disorders (back, neck and shoulders’ pain) among dental personnel in Jeddah–Saudi Arabia. Journal of Dental Health, Oral Disorders and Therapy. 2018;9(5):399-405.
- He L, Yue J, Yang L, Wu B, Cao G, Guo Y, et al. Cervicogenic headache alleviation after cervical coblationnucleoplasty: A prospective cohort study. Medicine. 2016;95(39).
- Kapitán M, Pilbauerová N, Vavřičková L, Šustová Z, Machač S. Prevalence of musculoskeletal disorders symptoms among Czech dental students. Part 1: a questionnaire survey. Acta Medica. 2019 Jan 22;61(4):131-6.
- Shimohata K, Hasegawa K, Onodera O, Nishizawa M, Shimohata T. The clinical features, risk factors, and surgical treatment of cervicogenic headache in patients with cervical spine disorders requiring surgery. Headache: The Journal of Head and Face Pain. 2017;57(7):1109-17.
- Çoban G, Çöven İ, Çifçi BE, Yıldırım E, Yazıcı AC, Horasanlı B. The importance of craniovertebral and cervicomedullary angles in cervicogenic headache.Diagnostic and Interventional Radiology. 2014;20(2):172.
- Lietz J, Ulusoy N, Nienhaus A. Prevention of musculoskeletal diseases and pain among dental professionals through ergonomic interventions: a systematic literature review. International journal of environmental research and public health. 2020 Jan;17(10):3482.
- Lietz J, Ulusoy N, Nienhaus A. Prevention of musculoskeletal diseases and pain among dental professionals through ergonomic interventions: a systematic literature review. International journal of environmental research and public health. 2020 Jan;17(10):3482.
- Narouze S. Cervicogenic headache. InEssentials of pain medicine 2018 Jan 1 (pp. 177-182). Elsevier.
The Ziauddin University is on the list of I4OA, I4OC, and JISC.
This is an open- access article distributed under the terms of the Creative Commons Attribution License (CC BY 4.0).
